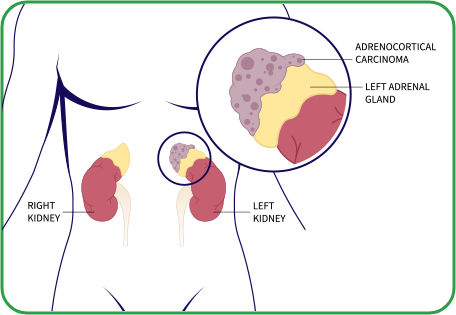
Adrenocortical carcinoma (ACC) is a rare cancer that forms in the outer layer of your adrenal glands, called the adrenal cortex. These glands sit on top of your kidneys and are part of your endocrine system. This means they make and release hormones. These hormones, called steroids, control many vital functions in your body.1,2
Two of the main hormones from the adrenal cortex are cortisol (also known as a glucocorticoid) and aldosterone (also known as a mineralocorticoid). These steroids help the body to maintain blood pressure, control metabolism (how your body uses food for energy), and respond to stress and illness.2
Adrenal cancer occurs when cells in the adrenal cortex mutate and grow out of control. Cancer cells can be present and form tumors in adrenal glands only (localized) or can spread (metastasize) to other parts of the body.1,3
Key Facts About ACC
What Is the Stage of My Tumor?4
Tumor sizes are often measured in centimeters (cm).
Adrenal cancers are often found after a person seeks treatment for the symptoms caused by the cancer. Some tumors are found when a doctor orders imaging tests for another condition.
There are 2 types of ACC tumors that can lead to signs and symptoms4:
About 6 in 10 patients (60%) will have a functioning tumor that produces high levels of hormones with symptoms that can include2
A nonfunctioning ACC tumor may not cause signs or symptoms in the early stage. The most common symptoms are1:
Many people do not receive a diagnosis of ACC until the cancer has spread beyond the adrenal gland. It is important to discuss any signs or symptoms with your doctor right away.
It is common for patients with excess hormones (functioning ACC) to also have Cushing’s syndrome.
This is caused by a buildup of cortisol over time.
Treatment for Cushing’s Syndrome related to ACC includes surgical removal of the tumor, when possible, and may also include administration of systemic therapies that work to reduce cortisol levels in the body (e.g., steroidogenesis inhibitors).
If your healthcare professional (HCP) suspects you might have ACC, your HCP will assess your medical history and order additional tests, such as:
Treatment will be based on the stage of the tumor, and whether the tumor is resectable (can be removed by surgery) or unresectable (cannot be removed by surgery).
If you have unresectable or metastatic disease, you may be treated with one or more of the following:
It is common for patients with excess hormones (functioning ACC) to also have Cushing’s syndrome.
This is caused by a buildup of cortisol over time.
Possible symptoms include:
Treatment for Cushing’s Syndrome related to ACC includes surgical removal of the tumor, when possible, and may also include administration of systemic therapies that work to reduce cortisol levels in the body (e.g., steroidogenesis inhibitors).
ACC care can be complex. The patient journey can involve not only a whole host of emotions, but also a whole range of tests, treatments, and HCPs. Treatment decisions should involve a multidisciplinary team (MDT) of experts.
Your treatment team may include
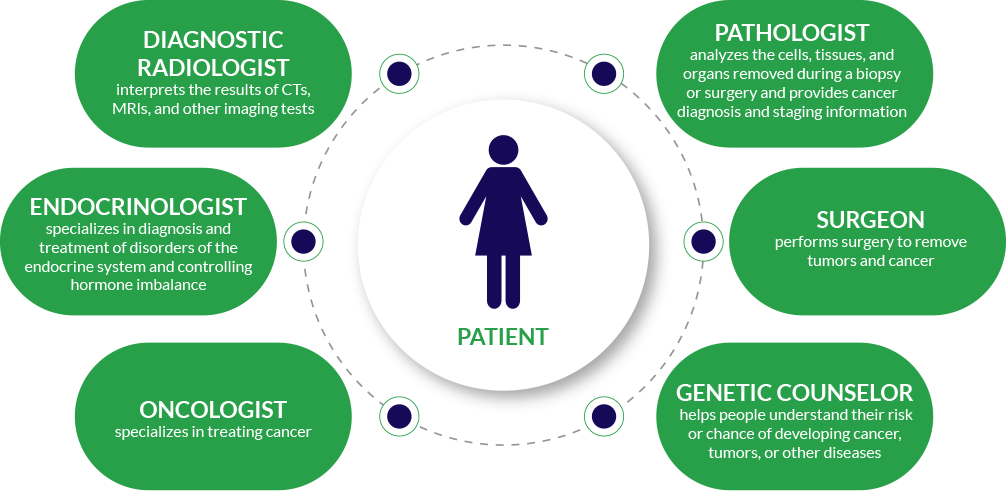
Each patient’s MDT is unique, and the above HCPs are only an example of the professionals that may be on your care team. There may be others, such as nurses, pharmacists, and psychologists who may provide care as part of your treatment plan.


Lysodren provides links to web sites of other organizations in order to provide visitors with certain information. A link does not constitute an endorsement of content, viewpoint, policies, products or services of that web site. Once you link to another web site not maintained by Lysodren, you are subject to the terms and conditions of that web site, including but not limited to its privacy policy.
Click the link above to continue or CANCEL